Safe by Todd Haynes
Todd Haynes wrote and directed the movie Safe in 1995. Julianne Moore plays the protagonist, Carol White, who experiences internal and external struggles with her surrounding environment.
Carol lives a fairly simple life: she gardens, runs errands, goes to the salon, and takes care of the home for her husband and stepson. While redoing her house, she begins to feel lethargic and sick. She visits a doctor, who finds nothing physically wrong with her, but refers Carol to a psychiatrist under the suspicion that her ailments are in her head. Slowly, her symptoms begin to worsen; she has a nosebleed at the hair salon, throws up before bed, and has a panic attack at a baby shower.
After an aerobic class, she sees a flyer about people struggling with symptoms similar to hers, leading her to believe she has severe environmental sensitivities.
After isolating herself from society to avoid the chemicals produced by everyday devices, she goes to the dry cleaners and seizes from visiting workers fumigating the store. While hospitalized, Carol sees an advertisement for Wrenwood, a community built to support people with environmental illnesses like hers, and decides to leave her life behind in the hopes Wrenwood would heal her. Unfortunately for Carol, her symptoms only got worse.
Towards the end of the film, Carol’s husband, Greg, moves her into an isolated igloo-like quarter as a final effort to improve, secluding herself from the rest of the community at Wrenwood.
The movie concludes with Carol saying “I love you,” after a director at Wrenwood suggested it might improve her condition. By finally loving herself, her true self, Carol can begin to recover mentally, physically, and emotionally. This movie displays the denial and lack of awareness people had regarding environmental and health issues. Overall, Carol’s environmental sensitivities were overlooked, illustrating the medical stances of people at the time the movie was filmed.


What is Multiple Chemical Sensitivity?
Multiple Chemical Sensitivity is defined as “the perhaps nonexistent ‘disease of modern civilization,’ said to be caused by reaction to many environmental contaminants” (Oxford University Press). In the 1940s and 1950s, there was a greater concern about food and environmental allergies (Shorter). This concern led people to believe that Multiple Chemical Sensitivity (MCS) was a descendent of a food allergy. In the 1940s, Dr. Theron Randolph introduced the illness as an “environmental illness” (The Journal of Allergy and Clinical Immunology 434). Dr. Randolph’s term debunked the idea that MCS was a food allergy. In the 1990s, Dr. Cullen coined the term Multiple Chemical Sensitivity, which is the term still used today (JACI 434). Another label often used is Idiopathic Environmental Intolerance, which suggests that the cause for these symptoms remains unknown (JACI 434). Unfortunately, not everyone believed that MCS was a real, medical illness; some believed it was a psychiatric or psychological illness (Johns Hopkins Medicine). The first case of MCS was reported in 1952 by Dr. Randolph; a woman came to him after being told she had hypochondria, yet her health was deteriorating and she could barely work (Xi Chen). The denial that this illness is real is what’s causing these detrimental effects on people.


People detoxify and eliminate chemicals differently, explaining why some might be more susceptible to diseases than others. (John Molot et al.1). High levels of exposure to chemicals have been historically known to cause childhood asthma, cancer, and blood and heart diseases (Isabella Clark 2). For patients with MCS, even low levels of chemical exposure can cause extreme symptoms (Abba I Terr 362). Everyday products like nail polish, ink, air fresheners, diesel and gasoline fumes, perfumes, hand sanitizer, hairspray, and even scented garbage bags can trigger a flair up (Cleveland Clinic). These everyday items that people are surrounded by make having MCS really hard.
Symptoms can be mild or have severe impacts on social and work life. These symptoms could be generally feeling unwell, runny nose, shortness of breath, burning eyes, paresthesia, confusion, fatigue, depression, memory loss, and heart issues (Molot et al. 2).
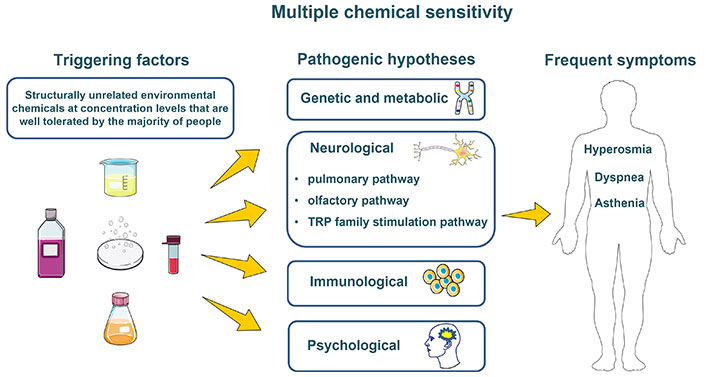
Unfortunately, there’s no real “cure.” The best form of treatment recommended by doctors is avoiding environmental chemicals (Terr 364). This could include self-isolation, a non-toxic lifestyle, or a reverse quarantine. In some cases, though, MCS is a psychological or psychiatric illness. In the case of it being a psychological or psychiatric disorder, a referral to a psychiatrist or psychologist is the best treatment (Karen E. Binkey).
At the time of the movie’s filming (1995), the discussion of MCS was increasingly being discussed. Dr. Cullen relabeled “environmental illness” as “Multiple Chemical Sensitivity” and the AIDS epidemic was at its peak. People were more aware of health crises, the environment, and medical limitations.
How Researching MCS Affects Our Understanding of Safe
By researching about MCS, the viewers are able to understand Carol in a deeper way. Now, the audience is able to better understand why Carol was reacting so severely to her makeup, gasoline fumes, and paint: she was not able to adequately detoxify the chemicals in her surrounding environment. Additionally, the audience can now see why Carol stopped visiting her friends, moved herself into a different room in the house, and eventually made the decision to go to Wrenwood: it was her form of treatment. Since no doctors were helping Carol, she took matters into her own hands, and made her own treatment plan. Unfortunately, since there is no real “cure” for MCS, she wasn’t getting much better.
Many people believed that she was faking her sickness, which is a common belief that many had regarding “invisible” illnesses. At Wrenwood, one of the patients said “First, I got sick and my husband thought I was crazy, and then he got sick the same way.” Like this woman, Carol’s husband did not fully believe the extent of her sickness, and he even said, “What the hell is going on here, huh?”
Additionally, Carol’s doctor sent her to a psychiatrist, thinking that her illness was mental and not physical. He says “You are perfectly healthy. You might want to consult someone.” The disbelief of doctors and people illustrates the medical limitations at the time the movie was filmed. While the doctor really might have thought Carol was healthy, the medical resources in 1995 were not advanced enough to see that Carol truly was very ill, and that it was not in her head. It can also be possible that a reason Idiopathic Environmental Intolerance was identified and named was because of its unknown origin: was MCS a physical or mental illness?
Research changes the initial, negative opinion of the movie and Carol. At first, many viewers might have thought that Carol was crazy, that she was faking her symptoms to get attention from her inattentive and skeptical husband. But by the end of the movie, and by researching, the audience might change their negative opinion to a positive one.
Works Cited
Binkley, Karen E. “Multiple Chemical Sensitivity/Idiopathic Environmental Intolerance: A Practical Approach to Diagnosis and Management.” The Journal of Allergy and Clinical Immunology: In Practice, vol. 11, no. 12, 2023, pp. 3645–3649. https://doi.org/10.1016/j.jaip.2023.08.039.
Chen, Xi. “Allergic to the World: Can Medicine Help People with Severe Intolerance to Chemicals?” The Guardian, 20 Sept. 2022, www.theguardian.com/lifeandstyle/2022/sep/20/allergic-to-the-world-multiple-chemical-sensitivity-mcs-can-medicine-help.
Clark, Isabella. “When Avoiding Chemicals Means Avoiding Others: Relational Exposures and Multiple Chemical Sensitivity.” Social Sciences, vol. 13, no. 10, 2024, p. 528. https://doi.org/10.3390/socsci13100528.
Cleveland Clinic. “Is Multiple Chemical Sensitivity a Real Thing?” Cleveland Clinic, 2 June 2025, my.clevelandclinic.org/health/diseases/multiple-chemical-sensitivity.
Johns Hopkins Medicine. “Multiple Chemical Sensitivity.” Johns Hopkins Medicine, www.hopkinsmedicine.org/health/conditions-and-diseases/multiple-chemical-sensitivity. Accessed 10 Dec. 2025.
Molot, John, et al. “Multiple Chemical Sensitivity: It’s Time to Catch Up to the Science.” Neuroscience & Biobehavioral Reviews, vol. 151, 15 May 2023, pp. 1–25. https://doi.org/10.1016/j.neubiorev.2023.105227.
“Multiple Chemical Sensitivities or Idiopathic Environmental Intolerances: Psychophysiologic Foundation of Knowledge for a Psychogenic Explanation.” Journal of Allergy and Clinical Immunology, vol. 99, no. 4, 10 Jan. 1997, pp. 434–437. https://doi.org/10.1016/S0091-6749(97)70066-6.
Porta, Miquel. “Multiple Chemical Sensitivities.” A Dictionary of Public Health, edited by John M. Last, Oxford University Press, 2018. Oxford Reference. Accessed 10 Dec. 2025. https://www.oxfordreference.com/view/10.1093/acref/9780191844386.001.0001/acref-9780191844386-e-2949
Safe. Directed by Todd Haynes, Sony Pictures Classics, 1995.
Shorter, Edward. “Multiple Chemical Sensitivity: Pseudodisease in Historical Perspective.” Scandinavian Journal of Work, Environment & Health, vol. 23, suppl. 3, 1997, pp. 35–42.
Terr, Abba I. “Multiple Chemical Sensitivities.” Journal of Allergy and Clinical Immunology, vol. 94, no. 2, 1 Aug. 1994, pp. 362–366. https://doi.org/10.1053/ai.1994.v94.a56015.



